MRI | Clinical Context | Mechanical Low Back Pain
MRI | Clinical Context | Mechanical Low Back Pain
MRI | Clinical Context | Mechanical Low Back Pain
MRI | Clinical Context | Mechanical Low Back Pain
MRI Integration
The MRI does not dictate our conclusions. It provides context. It can confirm. It can clarify. And occasionally it’s corrects our working hypothesis.
All the images presented on this page are of actual, successful patients. Read about their story on our testimonials page.
Risk of Misdirection
A heavy reliance on MRI findings can lead clinicians to prescribe one-size-fits-all protocols, or offer generic advice based on what looks abnormal, rather than taking the time to test what actually triggers your pain and prescribe a precise plan based on those findings.


What an MRI can actually tell us, and what it can't.
If you’ve had back pain for months or years, chances are you’ve already had one, maybe several, MRIs.
You’ve probably been told you have:
-
Disc degeneration
-
Bulging discs
-
Arthritis
-
Stenosis
-
A tear
-
“Wear and tear”
-
"Non-specific low back pain"
And yet… you still hurt. Here’s the important part:
-
An MRI does not tell us why your back hurts.
-
It shows structure, and that's it.
-
An MRI does not show how your spine behaves when for instance, you pick up your kids, sit at your desk, or rolling over in bed.
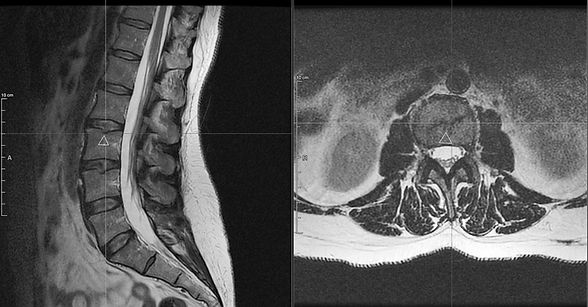
Remarkably many people have “abnormal” MRIs and no pain — like the image of one of our successful student-patient, to the left — and others have severe pain with relatively mild imaging findings — like the image below, also successful student-patient!
Three Ways Imaging Strengthens the Assessment
When combined with a proper physical examination, MRIs can help confirm, clarify, or even correct our working hypothesis, so we arrive at a more precise plan.
How MRIs Fit in the McGill Method Assessment?
In short, the sequence of events matters.
A proper McGill Method assessment for mechanical low back pain starts with:
-
A detailed review of both your medical history and your pain history
-
We spend an unlimited amount of time listening to your story and understanding your lifestyle, occupation, and home demands.
-
We individualize a physical exam to identify:
What movements trigger your pain
What postures rev up your symptoms
What loads you can tolerate and those you cannot
What daily demands keep picking the scab
What lifting technique errors need to be corrected
What role will walking play in your recovery
Only after we understand how your pain behaves do we look at your MRI—this order is critical.
At that point, the MRI becomes useful for three reasons:


#1 Images can confirm what we already suspect.
If your testing shows you’re sensitive to bending forward and your MRI shows a disc injury—that lines up.
If extension lights you up and we see significant canal narrowing or signs the facet joints are being irritated—that lines up.
If a sudden jolt of compression—like unknowingly stepping off a curb and landing stiff-legged—causes a sharp, boring pain in your back and we see evidence of an endplate injury—that lines up.
The MRI doesn’t diagnose you; it confirms the story your body already told us.
That builds confidence for both of us.
The order is critical!
Only after we understand how your pain behaves do we look at your MRI.
At that point, the MRI becomes useful to our mechanism-based clinical reasoning.
#2 Images help us estimate tissue sensitivity.
Some tissues calm down quickly. Others stay reactive longer. When the imaging suggests a structure that’s slower to settle—or easier to re-irritate—we plan your progression with tighter guardrails.
Your MRI helps us better estimate:
-
How quickly we can progress your loading
-
How much recovery time you may need between exposures
-
How wide your “buffer” is before symptoms spike
-
Which movements and loads require more precision early on
That’s not a fear-based approach. This is intelligent planning.

The value an MRI adds to the clinical picture
MRI doesn’t diagnose you; it confirms the story your body already told us.
That builds confidence for both of us.

#3 Images can clarify why you haven't improved yet.
Many people come to us saying:
“I’ve done PT.”
“I’ve had injections.”
“I rest when it hurts.”
“Nothing sticks.”
Sometimes the MRI reveals:
-
An injury that keeps getting re-irritated
-
A structural narrowing that makes certain movements risky
-
A stability issue that hasn’t been addressed
This isn’t meant to scare you or create fear. It’s meant to explain why a generic, image-driven treatment program didn’t solve the problem.
This isn't a fear-based approach.
This is a precision assessment with tightly scoped,
individualized, treatment planning.
What we don't do.
We do not solely focus treating your MRI.
We do not chase words like “degeneration” or “bulge.”
We do not assume surgery because something looks abnormal.
We absolutely do not ignore your symptoms because the
MRI “isn’t that bad.”
Instead, your pain pattern leads and the image provides context.
Why this matters.
If you’ve been stuck in a cycle of:
MRI → Injection → Temporary Relief → Pain Returns
That’s because structure was treated, but mechanics were never fully understood.
We flip that script. We identify the mechanical trigger first. Then we use imaging to refine the plan, not dictate it.
That’s how you minimize flare-ups and start building resilience.

